1. Introduction to Pancreas Transplantation
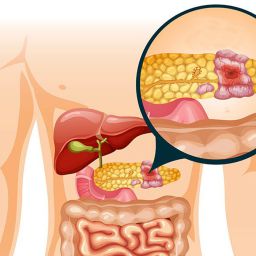
Pancreas transplantation is a surgical procedure in which a donor pancreas is implanted into a recipient whose pancreas is no longer functioning properly. It is most often performed for patients with type 1 diabetes and can be done either as a simultaneous pancreas-kidney (SPK) transplant (for patients with both diabetes and kidney failure) or as a pancreas-alone transplant (for patients who are only suffering from diabetes-related complications).
The goal of pancreas transplantation is to restore insulin production, thus eliminating the need for insulin injections and helping to regulate blood sugar levels. While this procedure offers significant improvements in quality of life for many patients, its success is influenced by a variety of factors, including genetic compatibility between the donor and recipient.
2. Genetic Factors in Organ Transplantation
In organ transplantation, genetic compatibility plays a critical role in ensuring that the transplanted organ is accepted by the recipient’s immune system. Several key genetic factors contribute to the success or failure of pancreas transplants, including:
- Human Leukocyte Antigen (HLA) Matching: HLA is a group of proteins found on the surface of cells that play a crucial role in the immune system’s ability to recognize and differentiate between self and non-self cells. Matching the HLA of the donor and recipient is essential to minimize the risk of rejection and improve the chances of transplant success.
- Blood Type Compatibility: Just as with HLA matching, blood type compatibility between the donor and recipient is vital for reducing the risk of organ rejection. Incompatible blood types can lead to the destruction of the transplanted organ by the immune system.
- Genetic Immune Response: The genetic makeup of both the donor and the recipient can influence the strength of their immune response, which may impact the rejection or acceptance of the transplanted pancreas. Certain genetic markers can determine the likelihood of immune tolerance or rejection.
3. The Role of HLA Matching in Pancreas Transplantation
The HLA system consists of various gene complexes that are important for the immune system to identify foreign tissues. For transplantation to be successful, the closer the match between the donor’s and recipient’s HLA genes, the lower the chances of the recipient’s immune system rejecting the transplant.
- HLA Class I and Class II: The immune system uses both Class I and Class II HLA proteins to detect foreign invaders like viruses or transplanted organs. For pancreas transplants, a high degree of HLA matching (for both Class I and Class II markers) significantly improves transplant success and reduces the need for heavy immunosuppressive drugs, which can lead to complications.
- The Significance of HLA Matching: Studies have shown that better HLA matching reduces the risk of acute rejection and long-term graft failure, enhancing the survival of both the pancreas and the patient. In cases where HLA mismatching occurs, the transplant may fail more quickly, requiring more intensive immunosuppression and higher medical risks.
- Impact on Pancreas Function: Proper HLA matching may also affect the long-term function of the transplanted pancreas, improving insulin secretion and reducing the chances of the pancreas becoming nonfunctional or failing altogether.
4. Genetic Conditions That Impact Pancreas Transplantation
Certain genetic conditions can impact both the success of pancreas transplantation and the recipient’s overall health, potentially complicating the procedure. These conditions may include:
4.1. Type 1 Diabetes (T1D)
While type 1 diabetes itself does not disqualify someone from receiving a pancreas transplant, it is the most common indication for the procedure. T1D is an autoimmune condition in which the immune system attacks the insulin-producing beta cells in the pancreas. Individuals with T1D who are undergoing pancreas transplantation need to be carefully screened for potential autoimmune responses that could increase the risk of transplant rejection.
- Genetic Predisposition to T1D: While the exact causes of type 1 diabetes remain unclear, genetic predisposition plays a significant role. Certain genes, particularly those within the HLA complex, are associated with an increased risk of developing T1D. Patients with these genetic markers may experience complications during the transplant process, including an increased risk of autoimmune rejection of the transplanted pancreas.
4.2. Cystic Fibrosis
Cystic fibrosis (CF) is another genetic condition that may impact pancreas transplantation. CF is caused by mutations in the CFTR gene, leading to thick mucus buildup in the pancreas and other organs. This condition can cause irreversible damage to the pancreas and often leads to diabetes, known as cystic fibrosis-related diabetes (CFRD).
- Complications in Pancreas Transplantation: Patients with cystic fibrosis may require a combined liver-pancreas transplant due to the liver damage that often occurs in CF patients. The presence of CFRD can also complicate the transplant process, as the genetic factors influencing the development of the disease may impact the likelihood of transplant rejection.
- HLA Considerations: The HLA matching process becomes particularly challenging for cystic fibrosis patients, as their genetic mutations can lead to immune system responses that increase the risk of transplant rejection.
4.3. Hemochromatosis
Hereditary hemochromatosis is a genetic disorder in which excessive iron is absorbed and stored in the body, leading to organ damage, including in the pancreas. This condition can cause diabetes mellitus and can be a factor in the decision to pursue a pancreas transplant.
- Impact on Pancreas Transplantation: In patients with hemochromatosis, iron overload can damage pancreatic tissue and impair insulin production. The presence of hemochromatosis in a pancreas transplant patient may increase the likelihood of complications, including rejection and dysfunction of the transplanted pancreas.
4.4. Genetic Syndromes and Organ Transplantation
Various rare genetic syndromes, such as Alström syndrome, MODY (Maturity Onset Diabetes of the Young), and Klinefelter syndrome, can impact pancreatic function and diabetes management. These syndromes may require a careful assessment of transplant eligibility, and special genetic considerations need to be made when determining the best course of action for the patient.
4.5. Mitochondrial Disorders
Mitochondrial diseases are inherited from the mother’s side and can affect various organs, including the pancreas. These disorders can cause dysfunction in insulin production and exacerbate complications in patients undergoing pancreas transplantation.
- Impact on Transplant Success: Mitochondrial disorders can lead to poorer outcomes after transplantation, as these conditions often cause damage to multiple organs, affecting overall health and recovery.
5. Genetic Testing in Pancreas Transplantation
Genetic testing plays an essential role in identifying patients who may be at higher risk of transplant rejection or complications. Genetic screening helps in determining:
- HLA Matching: Genetic testing is used to assess the compatibility of HLA markers between the donor and the recipient.
- Risk of Autoimmune Disorders: Genetic testing can help identify individuals who may be at an increased risk of autoimmune responses, such as in the case of T1D, where the immune system attacks the transplanted organ.
- Risk of Genetic Syndromes: Identifying genetic conditions that affect pancreatic function can help doctors understand the likelihood of transplant complications and prepare accordingly.
6. Preventive Measures and Management Strategies
6.1. Immunosuppressive Therapy
Immunosuppressive therapy is essential for preventing transplant rejection, but it must be carefully managed to avoid the side effects associated with these drugs. Genetic testing helps doctors determine the appropriate immunosuppressive drugs and dosages for patients based on their genetic predisposition to immune responses.
6.2. Ongoing Monitoring and Care
Regular monitoring of organ function, blood glucose levels, and immunosuppressive drug levels is crucial to ensuring that the pancreas transplant remains functional. Genetic testing can also be used to track the risk of rejection and to adjust treatment plans accordingly.
Genetic factors play a pivotal role in the success of pancreas transplantation. From HLA matching to genetic predispositions that affect immune responses, understanding these factors is critical to improving transplant outcomes. While genetic conditions such as cystic fibrosis, hemochromatosis, and type 1 diabetes can present challenges, advancements in genetic testing and immunosuppressive therapy allow healthcare providers to mitigate risks and enhance patient care.
By carefully considering genetic factors and tailoring treatment plans, the success of pancreas transplantation can be significantly improved, offering patients a new lease on life free from the burdens of insulin dependence and associated complications.