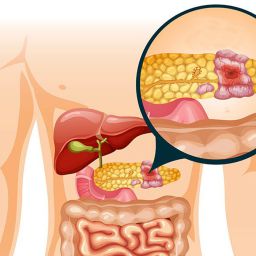
1. Introduction to Pancreas Transplantation
Pancreas transplantation is typically considered for individuals with type 1 diabetes who have severe complications such as kidney failure, frequent episodes of hypoglycemia (low blood sugar), or difficulty controlling blood sugar levels. A pancreas transplant can either be done as a standalone procedure or in combination with a kidney transplant, known as a simultaneous pancreas-kidney (SPK) transplant.
The surgery involves replacing a patient’s non-functioning pancreas with a healthy pancreas from a deceased donor. Once the transplant is successful, the patient’s body should be able to produce insulin naturally, eliminating the need for insulin injections or pumps.
However, like any major surgery, pancreas transplantation comes with significant risks. These risks can arise during the procedure itself or in the post-operative period, and they require careful management to avoid complications.
2. Risks Associated with Pancreas Transplantation
While pancreas transplants can offer great benefits, they come with a range of potential risks. These risks can be broadly categorized into immediate surgical risks, short-term complications, and long-term risks.
2.1. Immediate Surgical Risks
Any major surgery carries inherent risks, and pancreas transplantation is no exception. The most common immediate surgical risks include:
- Anesthesia Complications: As with any major surgery, anesthesia comes with risks such as allergic reactions, respiratory complications, or heart issues.
- Bleeding: Because pancreas transplantation is a major surgery that involves delicate organ manipulation, excessive bleeding may occur during the procedure, requiring blood transfusions or additional surgical interventions.
- Infection: Infection is a risk during any surgery, and the presence of a foreign organ increases the likelihood of infection. Both the surgical site and the transplanted organ itself are vulnerable to infections in the days and weeks following surgery.
- Blood Clots: During surgery, blood clots can form, potentially leading to deep vein thrombosis (DVT) or even pulmonary embolism (PE) if the clot travels to the lungs. Anticoagulant medications are often used to prevent clots.
2.2. Short-Term Risks After Pancreas Transplantation
Once the pancreas has been successfully transplanted, patients must remain vigilant for short-term complications that can occur as the body begins to adjust to the new organ.
- Rejection of the Transplanted Pancreas: One of the most significant short-term risks is organ rejection. Rejection occurs when the immune system recognizes the transplanted pancreas as foreign and attempts to destroy it. This is managed through the use of immunosuppressive medications, which can lower the risk of rejection but also increase susceptibility to infections and other complications.
- Infection: Immunosuppressive medications, which are necessary to prevent organ rejection, suppress the immune system and leave the patient more vulnerable to infections. These infections can be bacterial, viral, or fungal in nature and can affect various parts of the body, including the lungs, urinary tract, and surgical site.
- Pancreatic Complications: While rare, complications can arise with the transplanted pancreas itself, including issues with blood flow to the pancreas or problems with the organ’s function. Early complications may involve an inability of the pancreas to function properly, which may require a second surgery or an adjustment in immunosuppressive therapy.
- Gastrointestinal Issues: After pancreas transplantation, some patients may experience digestive issues such as nausea, vomiting, or diarrhea. These side effects are often caused by the medications and can be exacerbated by the adjustment period as the new organ begins to function.
2.3. Long-Term Risks After Pancreas Transplantation
The long-term risks of pancreas transplantation primarily relate to the ongoing need for immunosuppressive medications, which carry a variety of risks.
- Chronic Rejection: Over time, the immune system may continue to attack the transplanted pancreas, even with the use of immunosuppressive drugs. Chronic rejection can lead to a gradual decline in pancreatic function, requiring further interventions or even a second transplant.
- Increased Risk of Cancer: Immunosuppressive drugs increase the risk of certain types of cancer, particularly skin cancers and lymphomas. Patients who have undergone pancreas transplantation are often closely monitored for the development of cancers throughout their lifetime.
- Cardiovascular Risks: Long-term use of immunosuppressive drugs can lead to increased cholesterol and blood pressure levels, which in turn raise the risk of cardiovascular diseases. Patients who have received a pancreas transplant must manage their heart health vigilantly.
- Bone Health: Chronic use of immunosuppressive medications, particularly steroids, can lead to bone thinning (osteoporosis) and fractures. Patients may require medications or lifestyle changes to protect their bone health.
- Chronic Kidney Disease: While the pancreas transplant may alleviate the need for insulin therapy, the use of immunosuppressive medications can affect kidney function over time, potentially leading to kidney damage or even failure.
3. Prevention Methods After Pancreas Transplantation
While the risks associated with pancreas transplantation are significant, there are numerous preventive measures that can be taken to minimize the chances of complications and promote long-term success.
3.1. Close Monitoring and Regular Check-ups
One of the most critical aspects of post-transplant care is close monitoring of the patient’s health. Regular check-ups allow healthcare providers to detect complications such as rejection or infections early, improving the chances of successful intervention.
- Routine Blood Tests: Regular blood tests are crucial for monitoring the patient’s blood sugar levels, kidney function, and liver function. These tests can also detect signs of infection or organ rejection.
- Immunosuppressive Drug Monitoring: Blood levels of immunosuppressive drugs need to be carefully monitored to ensure that the patient is receiving the appropriate dosage. Too little medication increases the risk of organ rejection, while too much can make the patient more susceptible to infections.
3.2. Infection Prevention
Given the increased risk of infection due to immunosuppressive drugs, strict measures must be taken to prevent infections after a pancreas transplant.
- Prophylactic Antibiotics and Antivirals: Patients are typically given antibiotics or antiviral medications as a preventive measure to reduce the risk of infections during the early post-transplant period.
- Vaccinations: Vaccinations for preventable infections like influenza, pneumonia, and hepatitis are recommended to reduce the risk of infection.
- Personal Hygiene: Patients must practice good hygiene to prevent infections, particularly after surgery. This includes regular handwashing and care of the surgical site.
3.3. Managing Immunosuppressive Medications
Immunosuppressive medications are essential for preventing rejection but must be managed carefully to minimize side effects. Some prevention strategies include:
- Balanced Medication Regimen: Physicians must balance the use of immunosuppressive medications to provide adequate protection from rejection while minimizing the risk of side effects such as infections or cardiovascular complications.
- Alternative Medications: Newer immunosuppressive medications with fewer side effects may be prescribed to reduce risks such as cancer, diabetes, or kidney damage.
3.4. Lifestyle Modifications
Lifestyle changes can significantly reduce the risks associated with pancreas transplantation and improve overall health.
- Healthy Diet: A nutritious diet rich in fruits, vegetables, lean proteins, and whole grains is essential for overall health. Patients may also need to follow a specific diet to manage blood sugar levels and prevent weight gain caused by immunosuppressive drugs.
- Physical Activity: Regular exercise can help improve cardiovascular health, maintain a healthy weight, and improve overall well-being. Patients are often advised to start with low-impact exercises and gradually increase intensity as their recovery progresses.
- Smoking Cessation: Smoking can worsen cardiovascular health and increase the risk of complications. Patients are strongly encouraged to quit smoking as part of their recovery process.
3.5. Psychological Support
The emotional impact of undergoing a major surgery like a pancreas transplant should not be underestimated. Psychological support is vital in helping patients cope with the stress and emotional challenges of recovery, including anxiety about the transplant’s success, the impact of medications, and the adjustment to a new lifestyle.
Pancreas transplantation can significantly improve the quality of life for individuals with type 1 diabetes, especially those suffering from severe complications. However, like any major surgical procedure, pancreas transplants come with various risks. These risks include rejection, infections, long-term complications related to immunosuppressive therapy, and other health concerns such as cardiovascular issues and bone health.
The good news is that these risks can be effectively managed and minimized through regular monitoring, infection prevention strategies, careful medication management, lifestyle modifications, and psychological support. By taking these preventive steps, patients can significantly improve their chances of a successful transplant and enjoy a better quality of life post-transplant.