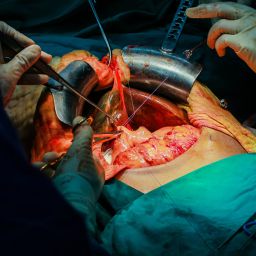
Introduction to Pediatric Liver Transplantation
Liver transplantation in children is typically performed when the child’s liver fails to function properly and cannot be treated by other medical means. The need for pediatric liver transplantation has grown due to various conditions such as genetic disorders, liver diseases, and viral infections. According to the Pediatric End-Stage Liver Disease (PELD) score, children with the most severe liver diseases are prioritized on the transplant waiting list.
The decision to proceed with a liver transplant is often based on the severity of the child’s liver condition, the progression of the disease, and the effectiveness of current treatments.
Common Indications for Liver Transplantation in Children
Liver failure in children can occur due to various causes, each necessitating a different approach to treatment and transplantation. The most common reasons for liver transplantation in children include:
1. Chronic Liver Disease
Conditions such as biliary atresia, cirrhosis, and chronic hepatitis can cause irreversible liver damage. For children with these conditions, liver transplantation may be the only viable treatment to restore liver function.
- Biliary Atresia: A congenital condition where the bile ducts are blocked or absent, leading to liver damage.
- Cirrhosis: Chronic liver disease causing scarring of liver tissue, making it difficult for the liver to function properly.
- Hepatitis: Chronic viral infections like hepatitis B or C, as well as autoimmune hepatitis, can lead to long-term liver damage.
2. Acute Liver Failure
Acute liver failure (ALF) can occur suddenly and requires immediate medical intervention. In children, ALF may result from viral infections, drug toxicity (such as acetaminophen overdose), or metabolic disorders. In severe cases, liver transplantation is needed to save the child’s life.
3. Metabolic Disorders
Genetic metabolic disorders, such as Wilson’s disease, alpha-1 antitrypsin deficiency, and familial amyloidosis, can cause liver damage. These diseases may lead to progressive liver failure, and liver transplantation can offer the only cure for some of these conditions.
4. Genetic and Congenital Liver Disorders
Some children are born with liver disorders that lead to early liver failure. Conditions such as galactosemia, tyrosinemia, and glycogen storage diseases may result in severe liver dysfunction that requires transplantation to preserve the child’s life.
5. Liver Tumors
Pediatric liver tumors, such as hepatoblastoma, may necessitate liver transplantation if the tumors cannot be surgically removed or if they are at an advanced stage.
The Liver Transplant Process for Children
The liver transplant process for children generally involves the following steps: evaluation, preparation, surgery, and post-transplant care. Each of these stages is carefully tailored to the child’s age, health status, and medical condition.
1. Pre-Transplant Evaluation
The first step in the liver transplant process is a thorough evaluation to assess the child’s eligibility for the transplant. This evaluation includes multiple tests and consultations with specialists in pediatric liver diseases, transplant surgeons, and anesthesiologists.
Tests and Diagnostics
Some of the tests and evaluations that are typically conducted before a liver transplant include:
- Blood Tests: To check liver function and determine blood type and compatibility.
- Imaging Tests: Ultrasound, CT scans, or MRIs to examine the liver’s size, condition, and the presence of any tumors.
- Liver Biopsy: A small tissue sample from the liver may be taken to examine the extent of damage and determine the cause of liver failure.
- Genetic Testing: To diagnose any underlying genetic or metabolic disorders.
- Cardiac and Pulmonary Evaluation: To ensure the child is fit for surgery and anesthesia.
- Nutritional Assessment: Nutritional status is important as children undergoing liver transplants may be malnourished, and nutritional support can improve recovery chances.
The evaluation will also assess other aspects of the child’s health, including their immune system function and any other medical conditions that may need to be managed during or after the transplant.
Psychosocial Assessment
Transplant teams will assess the child’s psychological and emotional health, as well as the support system available to them. This includes ensuring that the family understands the responsibilities post-transplant and is prepared for the long-term commitment involved.
2. The Transplant Waiting List and Organ Allocation
Once the child is approved for a transplant, they are placed on the transplant waiting list. The process of organ allocation in pediatric liver transplantation is managed by a national or regional organ-sharing network. In the United States, this system is regulated by the Organ Procurement and Transplantation Network (OPTN).
Liver transplantation in children is prioritized based on the Pediatric End-Stage Liver Disease (PELD) score, which takes into account the child’s condition, age, and severity of liver disease. Children with a high PELD score have a more urgent need for a transplant.
3. Finding a Suitable Donor
Liver transplants require a compatible donor liver, either from a living donor or a deceased donor. In children, finding a donor is especially challenging due to the size of the liver. Pediatric patients require a liver of the appropriate size for transplantation.
Living Donor Liver Transplantation
In some cases, a family member or close relative may be a suitable living donor. A living donor liver transplant involves removing a portion of the donor’s liver, which will regenerate over time. This option can help reduce the waiting time for a transplant, but it involves risks for both the donor and recipient.
Deceased Donor Liver Transplantation
In cases where a living donor is not available or suitable, children may receive a liver from a deceased donor. Deceased donor livers are allocated based on blood type compatibility, size match, and the urgency of the recipient’s medical condition.
4. The Transplant Surgery
Liver transplantation surgery in children is complex and typically takes several hours. The child is placed under general anesthesia, and the damaged liver is removed. The donor liver is then carefully implanted and connected to the recipient’s blood vessels and bile ducts.
Given that children are still growing, the surgical approach is often adjusted based on the child’s size and age. Pediatric transplant surgeons have specialized training in performing liver transplants on children to ensure the best outcome.
5. Post-Transplant Care and Monitoring
After the transplant, the child will be closely monitored in a specialized pediatric transplant unit. Key aspects of post-transplant care include:
- Immunosuppressive Therapy: To prevent organ rejection, the child will need to take immunosuppressive medications. These drugs suppress the immune system to avoid the body attacking the new liver.
- Nutritional Support: Children undergoing liver transplants may need nutritional support to promote healing and growth. Nutritional assessments will continue during recovery to ensure the child receives the necessary vitamins and minerals.
- Infection Control: Immunosuppressive drugs increase the risk of infections, so the child will be monitored for any signs of infection and receive appropriate treatment as needed.
- Routine Blood Tests: Blood tests are conducted regularly to monitor liver function, drug levels, and overall health.
- Follow-Up Visits: The child will require regular follow-up visits to assess liver function and check for signs of rejection or complications.
6. Long-Term Care and Lifelong Monitoring
After recovery, children who have undergone a liver transplant need lifelong monitoring and care. The first few years after a liver transplant are crucial as the child’s immune system adjusts to the new liver. Regular medical checkups and lab tests are necessary to ensure the liver remains healthy and functioning properly.
Special Considerations for Pediatric Liver Transplantation
Pediatric liver transplantation presents unique challenges and requires specialized care tailored to the child’s developmental and physiological needs. Some key considerations include:
1. Growth and Development
Liver transplantation in children must be carefully managed to ensure that the child’s growth and development are not hindered. Pediatric transplant teams work closely with endocrinologists and nutritionists to monitor the child’s growth and nutritional needs.
2. Age and Size Compatibility
As mentioned, liver size is a significant concern in pediatric liver transplantation. The donor liver must be the right size for the child’s body, which may involve the use of split livers or partial liver transplants in certain cases.
3. Emotional and Psychological Support
Children undergoing liver transplants, as well as their families, face emotional and psychological challenges. The transplant process can be overwhelming, and the child may experience anxiety, depression, or trauma. Providing psychological support and counseling is a crucial component of the transplant process.
4. Education and Support for Families
Families need to be educated about the process, the medications, the risks, and the long-term care involved in liver transplantation. Support groups and family counseling can be beneficial in helping families cope with the challenges of transplant life.
Liver transplantation in children is a complex, multifaceted procedure that requires careful evaluation, surgery, and lifelong care. It offers hope for children suffering from liver failure and provides a pathway to improved health and quality of life. However, the process is not without challenges, and it is essential to take special considerations into account, such as the child’s age, growth, and emotional well-being.
By understanding the processes involved and addressing the unique needs of pediatric patients, we can improve outcomes and ensure that children have the best chance for a healthy and happy future after liver transplantation.