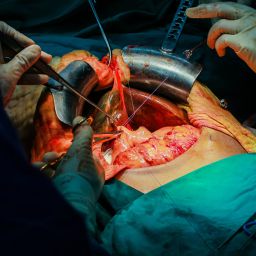
The First Year After Liver Transplant: A Crucial Period
The first year after a liver transplant is the most critical period for recovery. During this time, the body is adjusting to the new organ, and the risk of complications, such as organ rejection or infection, is heightened. Patients must follow a strict post-transplant care regimen, including regular check-ups, lab tests, and adherence to prescribed medications. However, this phase also presents an opportunity for long-term improvements in health and quality of life.
Physical Recovery and Rehabilitation
Recovery after a liver transplant requires a multi-disciplinary approach that includes physical rehabilitation. This process involves the gradual restoration of strength, stamina, and overall physical function.
1. Physical Activity and Exercise
Engaging in regular physical activity is vital for improving overall health after a liver transplant. Exercise helps with physical rehabilitation by strengthening muscles, improving circulation, and reducing fatigue.
- Start Slowly: Initially, the body may feel weak, and patients may experience low energy levels. It’s important to start with light activities, such as walking or gentle stretching.
- Gradual Increase in Intensity: Over time, as the body recovers, exercise intensity can be gradually increased. Low-impact exercises such as swimming, cycling, or yoga are excellent choices for transplant recipients.
- Regular Exercise Schedule: Consistency is key to maximizing the benefits of physical activity. A regular exercise routine, guided by a healthcare provider, helps patients regain their strength and avoid complications such as weight gain or loss of muscle mass.
2. Nutrition and Diet
Proper nutrition plays a significant role in the recovery process. After a liver transplant, patients must focus on consuming a well-balanced diet that promotes healing and supports long-term liver function.
- High-Protein, Low-Sodium Diet: After the transplant, a diet high in protein is essential for tissue repair and muscle maintenance. However, reducing sodium intake can help prevent fluid retention, a common issue in liver transplant recipients.
- Healthy Fats and Carbohydrates: Including healthy fats (like those from avocados, nuts, and fish) and complex carbohydrates (like whole grains, vegetables, and fruits) ensures a balanced diet that promotes healing.
- Avoiding Alcohol and Caffeine: Alcohol should be completely avoided, as it can put undue strain on the liver. Caffeine intake should also be minimized to avoid overstimulation and dehydration.
- Supplements: Patients may require additional supplements, such as vitamins and minerals, particularly vitamin D and calcium, to prevent bone density loss due to immunosuppressive medications.
3. Managing Medication Adherence
Immunosuppressive drugs are essential after a liver transplant to prevent organ rejection. However, these medications come with side effects, including increased susceptibility to infections, weight gain, and osteoporosis. Proper management of these medications is vital for enhancing quality of life.
- Strict Adherence to Medication Regimen: Patients must take their immunosuppressive drugs exactly as prescribed. Skipping doses or altering the dosage can increase the risk of rejection or other complications.
- Managing Side Effects: Some side effects of immunosuppressive drugs can affect the patient’s daily life. Working closely with a healthcare provider to adjust medications or manage symptoms such as weight gain, high blood pressure, and diabetes is crucial.
- Regular Monitoring: Blood tests are essential to monitor drug levels, liver function, and the patient’s overall health. Regular follow-up visits with the transplant team will ensure optimal medication management.
Psychological and Emotional Well-Being
Liver transplant recipients may face a range of emotional challenges after surgery. The physical changes, as well as the stress of living with a transplanted organ, can lead to feelings of anxiety, depression, and uncertainty.
1. Addressing Emotional Challenges
Psychological support is a vital aspect of post-transplant care. Liver transplant recipients often experience anxiety, fear of organ rejection, and the emotional burden of dealing with a chronic illness.
- Therapy and Counseling: Speaking to a therapist or counselor can provide support during the recovery process. Cognitive-behavioral therapy (CBT) has proven effective in addressing anxiety and depression following major surgeries like liver transplants.
- Support Groups: Joining a liver transplant support group can help patients connect with others who are going through similar experiences. These groups offer emotional support and practical advice on coping with post-transplant challenges.
- Stress Management: Learning stress management techniques such as deep breathing, meditation, or mindfulness can be incredibly helpful in reducing anxiety and enhancing emotional well-being.
2. Mental Health and Cognitive Function
Liver transplant patients may experience cognitive changes, including memory issues or difficulty concentrating. These can be due to medications, hospitalizations, or the stress associated with transplant recovery.
- Mental Stimulation: Engaging in mentally stimulating activities, such as puzzles, reading, or learning new skills, can help maintain cognitive function.
- Routine and Structure: Having a daily routine can provide patients with a sense of stability and control, reducing feelings of anxiety and improving mental clarity.
Social Support and Rebuilding Relationships
Rebuilding social connections and strengthening relationships is an essential component of improving quality of life after a liver transplant. Patients may have had limited social interactions during their illness, and recovery offers an opportunity to reconnect with loved ones and friends.
1. Family Support
Family members play an integral role in the recovery process. Providing emotional support, helping with daily tasks, and attending medical appointments are all essential ways in which family members can assist a transplant recipient.
- Open Communication: It is important for patients and their families to engage in open and honest conversations about recovery goals, feelings, and any concerns they may have.
- Involving Family in Care: Family members can be involved in medication management, dietary planning, and organizing transportation for doctor visits, ensuring that patients have a strong support system during their recovery.
2. Returning to Work and Social Activities
As patients regain their strength and improve physically, returning to work and engaging in social activities becomes an important part of enhancing quality of life.
- Gradual Return to Work: Patients may feel ready to return to work after a period of recovery. It is important to do this gradually and with the support of their healthcare team to ensure they don’t overexert themselves.
- Socializing and Hobbies: Engaging in social activities, whether it be spending time with family or participating in hobbies, can provide emotional fulfillment and a sense of normalcy.
Prevention of Complications and Regular Health Monitoring
Preventing complications is key to maintaining a high quality of life after a liver transplant. Liver transplant recipients are at higher risk for infections, organ rejection, and chronic conditions related to immunosuppressive drugs.
1. Preventing Infection
Infection prevention is a critical aspect of post-transplant care. Patients are vulnerable to infections due to their immune-suppressing medications.
- Hand Hygiene: Regular hand washing is one of the simplest and most effective ways to reduce the risk of infections.
- Vaccination: Patients should stay up to date on recommended vaccinations, such as the flu vaccine, hepatitis B vaccine, and pneumococcal vaccine.
- Regular Monitoring for Signs of Infection: Patients should be educated about the symptoms of infections and encouraged to seek medical attention promptly if they notice signs like fever, chills, or unusual fatigue.
2. Monitoring for Organ Rejection
Regular check-ups and lab tests are necessary to monitor for signs of organ rejection. These tests include blood tests, imaging studies, and biopsies.
- Signs of Rejection: Patients should be aware of the early symptoms of organ rejection, which may include fever, fatigue, jaundice, or dark urine. If any of these signs appear, it is crucial to contact the healthcare team immediately.
3. Preventing Long-Term Complications
Transplant recipients are at higher risk of developing chronic conditions such as high blood pressure, diabetes, or osteoporosis due to immunosuppressive medications. Ongoing monitoring and lifestyle adjustments can help manage these risks.
Improving quality of life after a liver transplant requires a comprehensive approach that addresses physical recovery, emotional well-being, social support, and the prevention of complications. By focusing on exercise, diet, medication adherence, mental health, and ongoing monitoring, liver transplant recipients can significantly enhance their quality of life and enjoy a fulfilling, healthy future.
The road to recovery may be long, but with the right strategies in place, liver transplant patients can not only survive but thrive in their post-transplant life. Through a combination of medical care, lifestyle changes, and emotional support, individuals can regain their strength, enjoy greater well-being, and lead an active, engaged life.